Mid & Long term Vascular Access & Imaging Equipements for COVID-19 patients
To treat the severe complications of COVID-19, healthcare professionals require reliable vascular access devices and PPE for the safe administration of drugs such as antimicrobials, vasopressors, and other fluids. The 5th of April, the GAVECELT association (Italian Society of Central and Long term Venous Access) has published its considerations on the use of vascular access devices in patients with COVID-19 and some practical recommendations based on clinicians’ experiences and recent scientific literatures. Please see below some extracts and according Vygon products among the IntraVascular Therapies range:
Choice of peripheral venous access
“Patients with suspected or confirmed diagnosis of COVID-19 – but who do not require hospitalization in the ICU – can be initially treated with a peripheral venous access, which will be used for hydration and supportive therapies, but using this access – however – only to infuse drugs and solutions compatible with the peripheral venous route […]. These patients also need repeated blood samples. […]. In some COVID-19 patients Midline catheters may be recommended […]: (a) due to their long life, they reduce the number of peripheral venous access positioning maneuvers […]; (b) they allow high flow infusions; (c) they allow blood sampling […] (d) Midlines can be easily replaced over guidewire with a peripherally inserted central catheter (PICC) if indicated.”
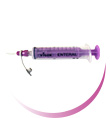
Midlines suitable for peripherally compatible infusates for a dwell time up to 29 days, Midline catheters avoid using several peripheral catheters and thus reduce repeated cannulations and manipulations.
- Lifecath Midline (1296.xxx): from 3F to 5F; 20 cm or 25 cm long; 1L and 2L. See the brochure
- Smartmidline (128.xxx): up to 5F; preferably 12 cm, 15 cm and 20 cm; 1L. Quick and easy insertion technique (Seldinger technique). Compatible with CT-scan. See the brochure
Choice of central venous access
“The COVID patient requiring hospitalization in intensive care unit needs a central venous access for several reasons: multiple and high-flow infusion therapies, administration of vasopressor drugs and other drugs not compatible with the peripheral route, parenteral nutrition, hemodynamic monitoring, repeated daily blood samples. […] Recently, several studies have highlighted the potential benefits of using peripherally inserted central catheters (PICC), if power injectable and in polyurethane (non-valved, open-ended) in intensive care unit. In the acutely ill patient with COVID-19, the use of these devices -especially if double-lumen (5Fr) and triple lumen (5Fr or 6Fr) – may be particularly suitable […]:
- the insertion of a PICC is completely free of risk of pleuropulmonary complications (pneumothorax, hemothorax), which can be fatal in patients with COVID-19 pneumonia; […] ; does not require that the patient is in supine position (which may be impossible in some COVID-19 patients), but can also be performed in patients in a sitting position, and in extreme cases even in pronated patients
– in patients on non-invasive ventilation, keeping the neck free […] is undoubtedly an advantage in terms of managing respiratory therapy and venous access; - in tracheostomized patients, PICC management will be safer […], both for the patient (lower risk of contamination of the emergency catheter site) and the operator (lower risk of exposure to patient tracheal secretions);
- PICC has no contraindications even in the heavily anticoagulated patient;
- also, the insertion of a PICC leaves the venous vessels in the supraclavicular and inguinal area free for ECMO cannulation.”
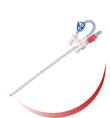
PICC lines for patients with COVID-19 requiring a central IV access for administrating several infusates, possibly with high osmolarity or extreme pH. Multilumen PICC lines allow simultaneous infusion of incompatible drugs (i.e. antibiotics, TPN …). Inserted peripherally, PICC lines keep the thoracic and neck area available in case ventilation is required. In the pronated COVID-19 patient, the dressing is easier to manage and kept away from the patient’s oral and tracheal secretions.
- Maxflo Expert (8394.xxx): from 4F to 6F; 1L, 2L, 3L. Maxflo Expert is a silver impregnated PICC thus very helpful to prevent microbial colonization. It is also compatible with CT-scan. See the brochure
- Lifecath PICC (1294.xxx): from 3F to 5F; 1L and 2L. See the brochure
Appropriate choice of insertion technique
“All central venous accesses (PICC, CICC, FICC) should of course be positioned by ultrasoundguidance, as recommended by all international guidelines : […] allowing (a) to choose the most appropriate vein, (b) to perform the venipuncture safely, (c) to exclude immediately some possible complications related to the puncture, (d) to verify the correct direction of the guidewire and/or of the catheter (tip navigation) and (e) to verify the correct final position (tip location). […] it is imperative to check the location of the tip of the central venous catheter by non radiological methods, such as intracavitary electrocardiography (IC-ECG) and transthoracic echocardiography (TTE). […] Tip location by IC-ECG can also be performed at bedside minimizing the risk of contamination: […].” “In order to reduce the risk of catheter-related venous thrombosis, in addition to the mandatory use of ultrasound-guided venipuncture, it should be verified that the size of the cannulated vein (brachial or basilica) is at least three times the external diameter of the Midline […]”
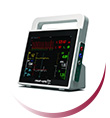
Vysion XS Ultra-Portable Ultrasound: useful for a pre-diagnostic in Emergency Department Emergency Care physicians can make a quick and reliable diagnosis of each patient’s situation and immediately choose the best treatment. Useful also for a safe insertion of IV lines. Ordering code (U-lite). See the brochure
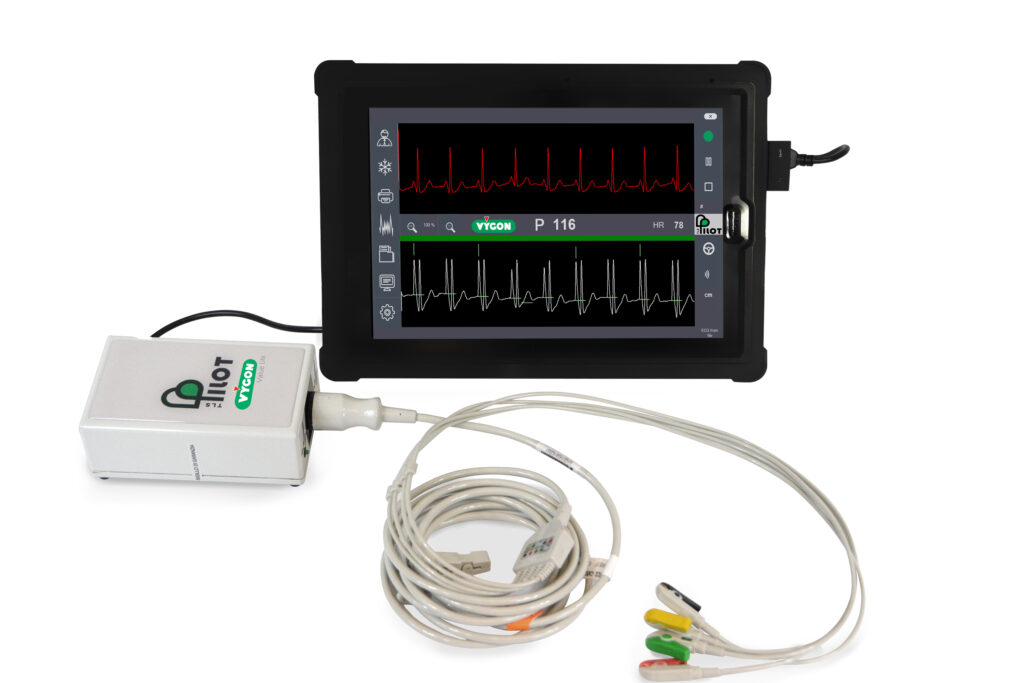
Pilot TLS ECG Catheter Tip Location System: useful for checking the tip location of central venous catheters. See the brochure
- Ordering code (TLSMF02).
Taking appropriate precautions to avoid operator contamination
“The insertion of central venous accesses or long term peripheral venous accesses should be performed following the CDC recommendations for vascular access in COVID-19 patients: For patient protection, the operator should take the highest ‘standard’ barrier precautions (hand hygiene before the maneuver, skin antisepsis with 2% chlorhexidine in 70% isopropyl alcohol, nonsterile surgical mask, non-sterile cap, sterile gloves, waterproof sterile gown, wide sterile field on the patient, sterile probe cover of appropriate length around the ultrasound probe). […]”
Maximum Barrier Procedure Sets (including PPE: gown, gloves, hat, surgical mask, full body drapes).
- PICC/Midline Max barrier VYSET (V02771818). See the brochure
If you are in need, please contact us for product availability at marketingbenelux@vygon.com.
You may also be interested in: