Haemodynamic patient management and vascular access for the COVID-19 patient in ICU
Recent information provided by ESICM, AVA, GaveCelt & KDOQI indicate an increased risk of vascular access complications for COVID-19 patients in the ICU. These include:
- Hypercoagulation. This appears to be a common factor which results in increased rates of venous thrombosis and catheter occlusion. In addition and despite treatment with heparin, clinicians are also experiencing premature failure of haemofiltration filters.
- Increased rates of CRBSi. This appears to be due to multiple factors including; increased ICU stay time > 5days, . Tthe presence of multiple iv access devices, placement of vascular access devices as an emergency procedure, increased frequency for iv line access, immunocompromised patients.
- Acute kidney injury (AKI). In general the rate of AKI has increased, with data ranging from 20 – 60% of the ICU patient population, when an average of 20-30% is typically expected in the general ICU population.
Fluid Management
Initial advice was to maintain a low fluid volume, however this has been changed to ‘optimise fluid volume status’ on arrival into the ICU and then to maintain a close control over fluids with all ARDS patients.
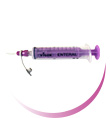
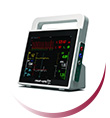
MostCare Up can assist with fluid patient management, by simply using the arterial pressure signal. Data is beat by beat and provides instant information to help guide patient management and avoid fluid overload. Unlike alternative technologies MostCare Up does not require calibration, which avoids the introduction of additional fluids into an already fluid challenged patient population. Simple use of the passive leg raise manoeuvre will also help guide the fluid management strategy, patient by patient. See the brochure
Additional Central Venous lumens or higher flow rate?
The indications are that the ARDS patients which represent ~ 50% of the current ICU population require more dedicated lumens. Whilst those patients with sepsis, ~ 25%, require both more lumens and high flow to improve haemodynamic circulation.
In addition we have seen a move towards using antimicrobial technology for insertion via the right internal jugular vein and when using non protected technologies a move towards insertion via the Axillary vein, to increase the distance from possible respiratory seeding of the catheter.
Catheter technology
Guidelines recommend the use of antimicrobial catheter technology when catheter dwell time is expected to exceed 5 days.
In addition to the risk factors listed above, placement of an antimicrobial catheter should be considered in the following circumstances; to limit catheter colonisation, which ultimately leads to CRBSi:
- If the previous CICC needs to be replaced
- If there was a previous episode of CRBSi or in case of sepsis
- If there is already a central venous catheter in situ
- When the patient has any type of implant
At Vygon we offer a choice of two antimicrobial catheter technologies, MultiStar & Multicath Expert. MultiStar is our 1st choice when dwell time is anticipated to be 5 days or longer.
Catheter placement and tip location (Combcard)
To ensure fast, safe catheter placement use ECG catheter tip location techniques such as Combcard or Vygocard. This avoids the need to transfer the patient for an x-ray and the time required for decontamination of X-Ray equipment.
Confirm the absence of a pneumothorax by using Ultrasound* See the brochure
Arterial Access
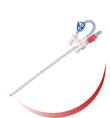
Hypercoagulation is causing multiple problems including increased rates of both venous and arterial catheter occlusion. Accordingly we are seeing a move away from radial placement towards femoral with 18g catheters like Leadercath, using the Seldinger insertion technique.
Haemodialysis catheter
Typically up to 30% of ICU patients were expected to present AKI and require some form of acute dialysis.
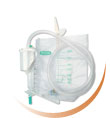
Initial reports from China indicated that AKI affected <10% of ICU patients, however recent European data indicates that AKI is experienced by >30% of the COVID-19 ICU population. In these patients it is advised to avoid left sided placement of vascular access devices and to reserve the RIJ for placement of a temporary haemodialysis 15cm catheter like Trilysecath or Dualysecath. See the brochure
For advice and guidance on product selection please email marketingbenelux@vygon.com.
You may also be interested in:
- Vygon Statement on the Covid-19 situation
- Mid & Long term Vascular Access & Imaging Equipements for COVID-19 patients
- Protection and intubation
- Non-invasive ventilation support
* Biasucci DG, La Greca A, Scoppettuolo G, Pittiruti M. What’s really new in the field of vascular access? Towards a global use of ultrasound. Intensive Care Med. 2015 Apr; 41(4):731-3.